Gene Therapy Targets Liver in Mouse MS Study
By LabMedica International staff writers
Posted on 03 Oct 2017
Results of studies carried out on a mouse model of multiple sclerosis (MS) demonstrated the potential of a novel potent and long-lasting gene immunotherapy approach for preventing and treating the disease.Posted on 03 Oct 2017
MS, which affects more than 200 million people worldwide, is an inflammatory disease in which the myelin sheaths around the axons of the brain and spinal cord are damaged by autoimmune attack, leading to demyelination and scarring as well as a broad spectrum of signs and symptoms.
Image: Researchers have found MS can be inhibited or reversed using a novel gene therapy technique that stops the disease’s immune response in mouse models (Photo courtesy of the University of Florida Health).
Researchers agree that MS could substantially benefit from an adeno-associated virus (AAV) immunotherapy designed to restore a robust and durable antigen-specific tolerance. However, developing a sufficiently potent and lasting immune-regulatory therapy that can intervene in ongoing disease has been a major challenge and has thus far been elusive.
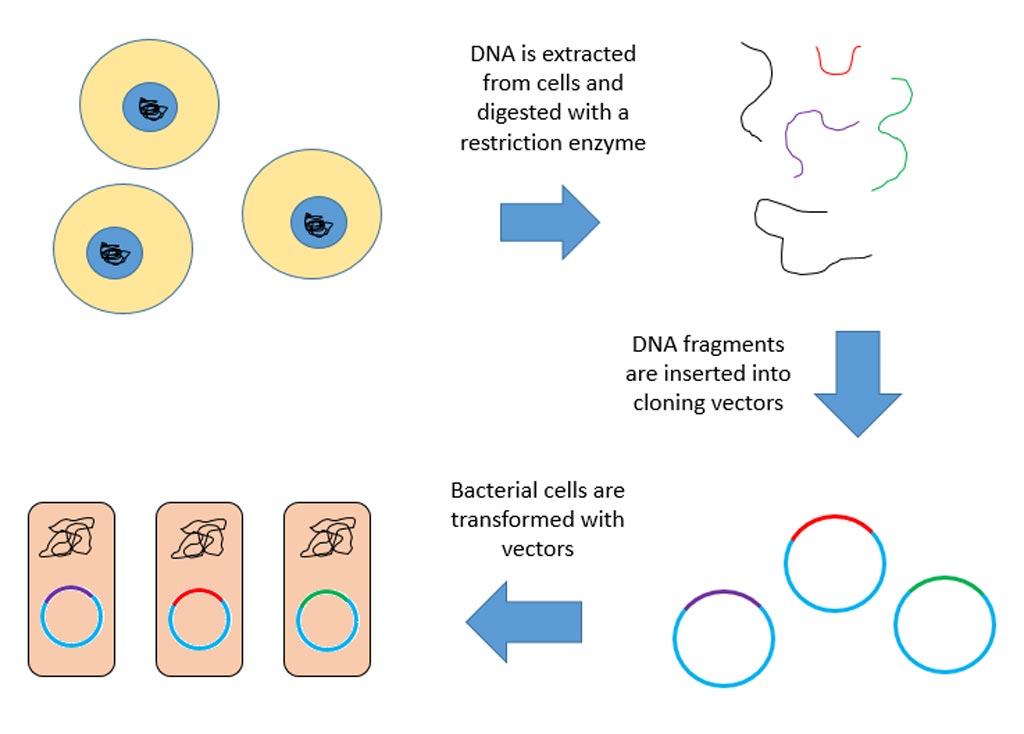
Investigators at the University of Florida (Gainesville, USA) addressed this problem by developing a highly effective and robust tolerance-inducing in vivo gene therapy. Using a pre-clinical animal model, they designed a liver-targeting gene transfer vector that expressed the DNA for programming the full-length myelin oligodendrocyte glycoprotein (MOG) in hepatocytes. This strategy capitalized on the unique ability of the liver to induce immune tolerance.
The investigators reported in the September 21, 2017, online edition of the journal Molecular Therapy that this powerful gene immunotherapy restored immune tolerance by inducing functional MOG-specific regulatory T-cells (Tregs) in vivo, independent of major histocompatibility complex (MHC) restrictions. They demonstrated that naïve mice were protected from developing the disease and neurological deficits. In addition, they demonstrated that when given to mice with preexisting disease, ranging from mild neurological deficits to severe paralysis, the gene immunotherapy abrogated central nervous system inflammation and significantly reversed clinical symptoms of disease.
When administered to mice with mild-to-moderate neurological deficits, the AAV vector alone was effective at reversing both clinical and pathological signs of disease. When combined with a short course of immune suppression, the AAV immunotherapy rescued mice from fatal end-stage MS and restored mobility to mice that had exhibited severe paralysis.
"Using a clinically tested gene therapy platform, we are able to induce very specific regulatory cells that target the self-reactive cells that are responsible for causing disease," said senior author Dr. Brad E. Hoffman, assistant professor of pediatrics and neuroscience at the University of Florida. "In contrast, most current therapies for autoimmune diseases such as multiple sclerosis are based on general immune suppression, which has various side effects or complications."
"Traditional AAV gene therapy has been focused on delivering a transgene that produces a therapeutic protein," said Dr. Hoffman. "Here we use the platform purposely to induce specific regulatory cells in order to restore immune tolerance and reverse an autoimmune disease. Our results are very promising. We have demonstrated that stable immune tolerance can be re-established and that active disease can be stopped and clinical symptoms reversed using our gene immunotherapy, especially during early onset of disease. Even though these studies were performed in a less complex mouse model, the data suggest this may be a potential therapy in humans with additional optimization."
Related Links:
University of Florida